Earl Baumgardner was told he had an aortic aneurysm, a weak spot in the wall of a major blood vessel that was stretching like a balloon and in danger of rupturing. He was told by some of the nation’s leading heart experts that a traditional open procedure was too risky and that nothing could be done. Then he was told about a procedure at UMass Memorial Health that could save his life.
THE INNOVATION THAT SAVED EARL
FEVAR: We’re one of 10 in the country providing it
Abdominal aortic aneurysm (AAA) is a life-threatening condition that occurs when part of the aorta that supplies blood from the heart to the rest of the body begins to stretch like a balloon and becomes weak. Eventually, if left untreated, it can rupture, and when that happens less than 10 percent survive. More than 200,000 Americans are diagnosed with AAA each year. And because the weak spot, or “balloon,” can sometimes occur in areas of the abdomen or chest that are difficult to reach for repair, some patients are told that nothing can be done.
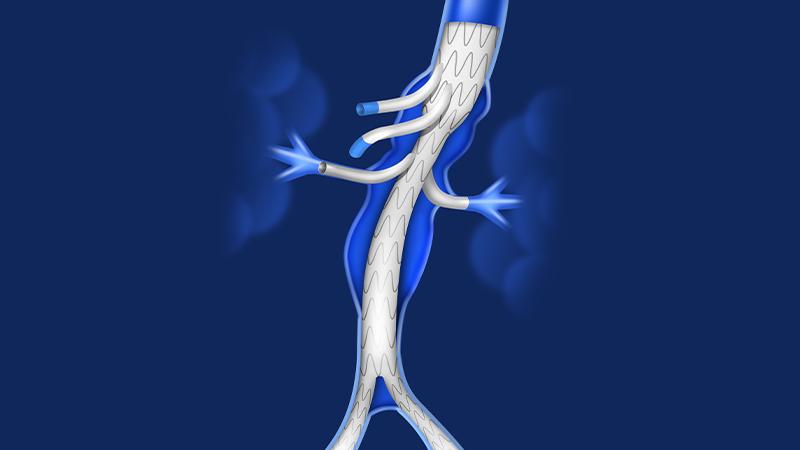
That’s where FEVAR and the team at UMass Memorial Health come in. FEVAR stands for Fenestrated Endovascular Aneurysm Repair. Simply put, FEVAR is a special type of surgical repair that requires our team to design a device that is placed into the aorta, thus allowing the blood to pass through this stent while excluding the aneurysm. But, in order to meet the special needs of the aorta, this device, called a fenestrated endograft, must be customized to match the exact physiology of each patient. Said another way, we use special imaging software that allows us to take exact measurements to match the specific anatomy. The endograft is designed just for that patient.
BENEFITS OF FEVAR
-
Avoid a large incision in the abdomen or chest resulting in a quicker recovery
-
A reduced risk of lung, heart or abdominal problems
-
Lower risk of complications
-
A shorter hospital stay
FEVAR vs. Open surgical repair of an abdominal aortic aneurysm
Open repair means that a large incision is used to open up the chest or abdomen, exposing the organs for visibility and access. FEVAR only requires small incisions, and the chest or abdomen remains closed. This means there is less healing for the body to do after surgery and a shorter recovery time.
During an open repair, if the aneurysm is in your chest, you’ll be placed on cardiopulmonary bypass (a pump that temporarily takes over the function of the heart and lungs during surgery). If the aneurysm is in your abdomen, clamps will be used to stop the blood flow through your aorta while a fabric tube is sewn to healthy tissue above and below the aneurysm. Smaller tubes will be sewn on to the graft and connected to the blood vessels that lead to the kidneys, intestines and liver. Once these connections are made, the clamps will be removed, and blood is allowed to flow back through the repaired aorta. These steps are not necessary with FEVAR.
Following an open procedure, you’ll need to spend several days in the intensive care unit followed by another three to 10 days in the hospital with an extended recovery period. Most patients will require some time in a rehabilitation hospital. It’s important to know that some patients don’t qualify for open surgery because of significant heart or lung disease, or previous abdominal or thoracic surgery. FEVAR patients will typically spend about two to five days in the hospital, and the majority of the time, are able to return home. Sometimes a short stay in a rehab facility is needed to regain strength.
Who is at risk for an abdominal aortic aneurysm?
- Men over 65 with a smoking history are at the highest risk for AAA.
-
Women over 70 also become more prone to develop AAA and are known to have a higher mortality for rupture.
-
A family history of the condition can double your risk.
-
People who have had aneurysms in other parts of the body, especially in the legs, are at increased risk.
-
Smokers. Ninety percent of those with abdominal aortic aneurysms have a history of smoking.
-
Lastly, the presence of high blood pressure, high cholesterol and obesity can increase your risk of AAA.
AAA symptoms
Unfortunately, AAAs oftentimes have no symptoms. However, for some, especially those with an AAA that is growing, you might feel:
-
A deep pain in your stomach or side that doesn’t seem to let up
-
Back pain
-
A pulse in the area of your navel
More to Explore
Want to Know More?
If you have an aortic aneurysm, speak with your primary care physician or cardiologist about a referral. In addition, UMass Memorial Health can help you understand your risks for an abdominal aortic aneurysm and help you find a specialist. To learn more about this investigational procedure, call 855-UMASS-MD, or visit UMMHealth.org/aneurysm.
Relentless Innovation at UMass Memorial Health
As one of the leading academic medical centers in the country, we take our mission of research, education and outstanding patient care seriously. And because we’re also charged with the health and health care of all people throughout Central Massachusetts, we maintain an intense focus on creating new and better ways to make health care available for all. A better experience. Better outcomes. Healthier lives. It’s what we live for.
